Haploidentical transplant is an advanced medical procedure that has transformed the treatment of serious blood disorders. It provides a solution for patients who need a stem cell transplant but are unable to find a fully matched donor. With recent advancements, this technique has become safer and more effective, offering hope to many patients worldwide.
What is a Haploidentical Transplant?
A haploidentical transplant is a type of stem cell transplant in which the donor is only a half match to the patient. This means that the donor shares about 50 percent of the genetic markers required for compatibility. In most cases, close family members such as parents, children, or siblings can serve as donors.
Traditionally, doctors preferred fully matched donors to reduce complications. However, due to limited availability of matched donors, haploidentical transplants have become an important alternative.
Why is Haploidentical Transplant Important?
Many patients with life-threatening blood disorders require a stem cell transplant as part of their treatment. Finding a fully matched donor can be difficult and time-consuming. In some cases, patients may not find a match at all.
Haploidentical transplant solves this problem by allowing doctors to use partially matched donors from within the patient’s family. This significantly increases the chances of finding a donor quickly and starting treatment without delay.
Conditions Treated with Haploidentical Transplant
Haploidentical transplant is commonly used to treat various hematological conditions. These include leukemia, lymphoma, aplastic anemia, thalassemia, and multiple myeloma. It is also used in certain inherited blood disorders and immune system diseases.
The procedure is often recommended when other treatments such as chemotherapy or medications are not sufficient to cure the disease.
Procedure of Haploidentical Transplant
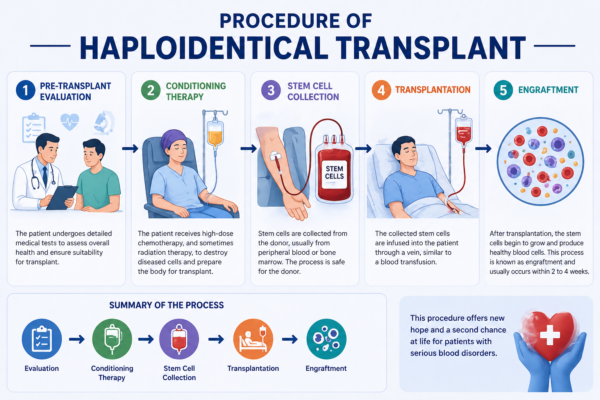
The process of haploidentical transplant involves several important steps.
Pre-Transplant Evaluation
Before the transplant, the patient undergoes a detailed medical evaluation. This includes blood tests, imaging studies, and assessment of organ function. The goal is to ensure that the patient is fit for the procedure.
Conditioning Therapy
The patient receives high-dose chemotherapy, and sometimes radiation therapy, to destroy diseased cells and prepare the body for the transplant. This step also suppresses the immune system to reduce the risk of rejection.
Stem Cell Collection
Stem cells are collected from the donor, usually from peripheral blood or bone marrow. The collection process is safe and does not cause long-term harm to the donor.
Transplantation
The collected stem cells are infused into the patient through a vein, similar to a blood transfusion. These cells then travel to the bone marrow.
Engraftment
After transplantation, the stem cells begin to grow and produce healthy blood cells. This process is known as engraftment and usually occurs within two to four weeks.
Advancements in Haploidentical Transplant
In the past, haploidentical transplants were associated with higher risks of complications. However, modern medical techniques have greatly improved outcomes. The use of better immune suppression methods and advanced supportive care has made the procedure much safer.
One of the major advancements is the use of post-transplant medications that help reduce complications such as graft-versus-host disease. These improvements have made haploidentical transplants comparable to fully matched transplants in many cases.
Benefits of Haploidentical Transplant
Haploidentical transplant offers several advantages. One of the biggest benefits is the availability of donors. Since family members can be used, most patients can find a suitable donor quickly.
It also reduces the waiting time for treatment, which is critical in aggressive diseases. In addition, it can be more cost-effective compared to unrelated donor transplants. Most importantly, it provides a potentially curative option for patients who otherwise have limited treatment choices.
Risks and Complications
Despite its benefits, haploidentical transplant carries certain risks. One of the main complications is graft-versus-host disease, where donor cells attack the patient’s body. Patients are also at risk of infections due to a weakened immune system.
Other complications may include graft failure, where the new cells do not grow properly, and side effects from chemotherapy or radiation. However, with proper medical care and monitoring, these risks can be managed effectively.
Recovery and Post-Transplant Care
Recovery after a haploidentical transplant is a gradual process. Patients require close monitoring during the initial weeks after the procedure. Regular blood tests and follow-up visits are necessary to track recovery.
Patients are advised to maintain good hygiene, follow a nutritious diet, and avoid exposure to infections. Medications are prescribed to prevent infections and manage complications. Full recovery may take several months, depending on the patient’s condition.
Who Can Undergo Haploidentical Transplant?
Not every patient is suitable for this procedure. Doctors evaluate several factors before recommending a haploidentical transplant. These include the type and stage of the disease, the patient’s overall health, and the availability of a suitable donor.
A detailed assessment by a specialist is essential to determine whether the procedure is appropriate.
Future Scope of Haploidentical Transplant
The future of haploidentical transplant is promising. Ongoing research is focused on improving success rates and reducing complications. Advances in immunotherapy and targeted treatments are expected to further enhance outcomes.
With continued progress, haploidentical transplant is becoming a widely accepted and reliable treatment option across the world.
Conclusion
Haploidentical transplant has significantly advanced the treatment of serious blood disorders by making stem cell transplantation accessible even without a fully matched donor. With improved techniques, better safety protocols, and higher success rates, this procedure offers a strong chance of recovery and long-term survival for many patients.
However, the success of a haploidentical transplant largely depends on timely diagnosis, proper patient selection, and expert medical care. Consulting the best hematologist ensures accurate evaluation, advanced treatment planning, and comprehensive post-transplant care, which are essential for achieving the best possible outcomes.

